A credentialed provider in the healthcare sector is someone who has been vetted by insurance companies or networks with all background information along with verification of the required credentials that enables the provider to offer a specific healthcare service in the industry.
Your Trusted Patner
Techera Med Systems is a medical billing company that offers full-service medical billing.
Services We Offer
Get an Appointment
Call Us Today for the Best Medical Billing Audit Service in the USA by Techera Med Systems
Get A Detailed MEDICAL BILLING AUDIT For Healthcare Practices
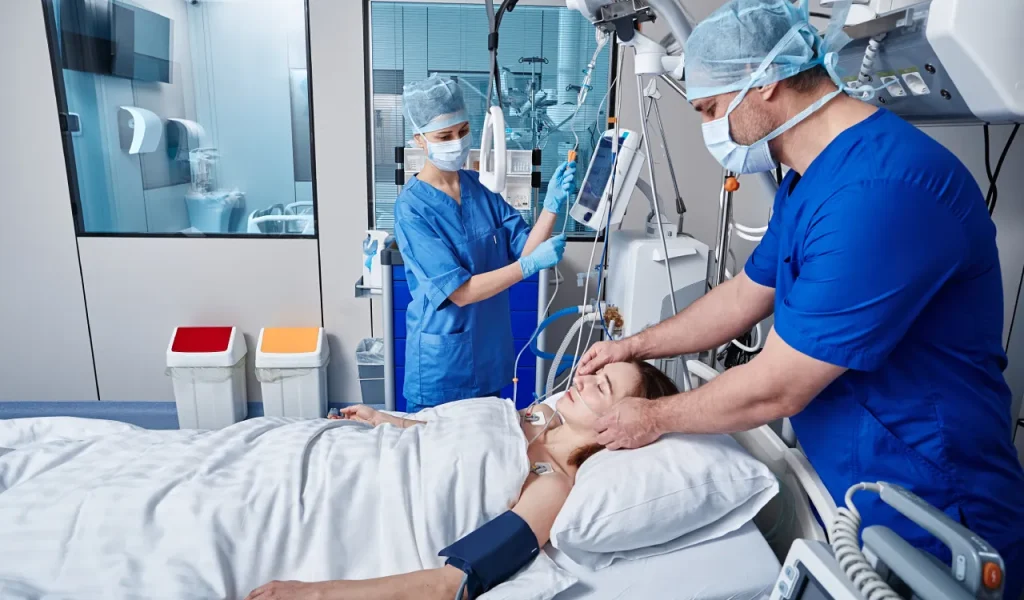
Simplify medical billing audits across all your departments by partnering with leading medical billing providers and coding partners for 24-hour medical billing services. When it comes to documentation or other audit-related tasks, there’s no fuss because we handle patient data securely.
Moreover, medical billing audits enhance and strengthen billing and coding processes, ensure stricter claims processes, and demonstrate that all necessary measures are in place to avoid future errors. Plus, ensure proper revenue cycle management (RCM) processes are set to increase income.
Our expert medical billing audit team consists of compliance officers, finance managers, case managers, IT, medical advisors, and HIMs. They ensure that the medical practices can not only meet regulatory requirements but also streamline processes and workflows to ensure higher profits through the claims process in the most rigorous and efficient way.





What Is A Medical Billing Audit?
A medical billing audit is a process performed to evaluate clinical documents, verify the accuracy, reliability, and validity of records maintained by medical facilities, and review billing documents submitted to taxpayers. Auditing allows for the detection, monitoring, and correction of inappropriate billing practices.
A medical bill audit is a complex process. You will need to manage many data sources, including clinical records, financial records, accounting documents, and policy-related documents. Therefore, it is very important to gather all the information in one system and arrange it correctly.
Medical Billing Audit Types
Medical billing audits and medical billing claims are available no matter the size of your business. Conducting regular audits can help ensure that your medical billing system is efficient and has sufficient cash flow. These are some of the types of reviews that are done in the medical field:
Sampling Audit
Conduct medical billing audits this way and select claims based on insurance funds that cover both small and large claims. Perform an audit. The focus is on dollar amounts, not the number of shares being analyzed. A random audit doesn’t mean you’ll receive a refund from your insurance company, but it may help complete a more thorough audit review.
Full Audit
The review is extensive and examines claims that have previously been audited manually or electronically. Additionally, it allows you to make claims to the claims administrator, which is the main goal of auditing.
Hybrid Medical Billing Audit
Hybrid medical billing audits combine random sampling audits with comprehensive audit reviews to achieve results including chargebacks and compliance. Additionally, it focuses on recovering overpayments quickly.
The Medical Practice Audit Process

Medical Billing Audits are considered to be crucial for the operational and financial performance of a medical practice. The process is rather simple, yet complicated because of several factors contributing to a smooth revenue cycle for medical practices.
An Internal Medical Billing Audit is highly involved in the financial affluence of medical practices as it gauges the strengths and weaknesses of the practice in order to improve its performance. Medical practices can simply type “medical practice audit companies near me” to find a quality billing company that can carry out an audit and help improve their revenue collections and decrease account receivables.
Your Practice is in Secure Hands!
Yes, Medical Practices! With Techera Med Systems, your RCM billing audit is in safe hands. We are a completely professional and HIPAA-compliant billing company that ensures data protection. This is why it is always a good idea to outsource your billing audit to our medical billing auditors who will provide you with an eagle-eyed view of your medical practice.
With our audit services, you can grow your practice without worrying about revenue leakages destroying your revenue collection rates.
Medical Billing Audits Made Secure with HIPAA Compliance
The Medical Billing Audit process is a good way to see the bigger picture when it comes to your medical practice and its overall performance. It allows you to fix all revenue leakages and contribute to better revenue cycle management.
However, for medical practices, these medical billing audit templates have to be outsourced to those RCM billing companies that are completely HIPAA compliant and ensure the protection of Private Healthcare Information (PHI). As a result, your medical practice can benefit from the audit while staying assured regarding the security of your patient’s healthcare information.
The RCM Medical Billing Audit Checklist
An audit checklist is essential for a billing and audit company to navigate the entire process. It helps in tracking all possible revenue leakages and contributes to a better revenue cycle. This is why medical billing audits are highly critical to ensure the accuracy as well as integrity of billing practices and to prevent revenue loss and financial distress.
Checklist:
Initially, search and verify the valid patient IDs.
Verify that all the patient demographic information is accurate and complete.
Ensure that the correct coding and billing of services are executed.
Review the accuracy of all insurance information and payment processing.
Ensure that claims are submitted within the required deadline.
Check for duplicate billing and proper use of modifiers.
Verify the appropriateness of documentation supporting the services billed.
Ensure that all applicable adjustments or discounts are implemented accurately.
Evaluate ethical and legal compliance with local, state, and federal regulations in order to avoid any kind of litigation.
Thus, we can say that a regular medical billing audit offers many benefits, such as improved revenue cycle management, compliance with legal rules, and low account receivables. As a result, increased financial stability for healthcare providers is ensured along with higher patient satisfaction.

Benefits to Hire Techera Med Systems
Enhanced cash flow
99% Claim Rate
Minimize A/R delays
Starts from 2.95% of your collections
EHR Flexible Solutions
Dedicated Team of 1000+ Experts
Frequently Asked Questions
What is the difference between enrollment and credentialing for a medical provider?
Fundamentally, credentialing refers to the formal validation of a medical or healthcare provider in a specific private health plan and enabling the provider to get the approval to join the network. On the other hand, the act of enrollment refers to the process through which a provider requests participation in a health insurance network.
What is the average duration of time needed to complete the credentialing process?
The standard duration to complete the credentialing process takes on average 90 to 120 days. However, if you hire credentialing experts from the billing sector, you can reduce the time frame to less than 90 days as well.
What is a credentialed provider?
What is the difference between credentialing and privileging?
Privileging includes a health care facility, for instance, a hospital authorizing providers to practice specific kinds of medicine and carry out procedures accordingly on the premises of the facility. As opposed to this, the credentialing process involves regulating and checking the licenses and certificates of the medical providers. The goal here is to check whether the credentials are in good standing or not, and evaluate if the medical practitioner is licensed to practice in the health care facility.

